OpenAI and Anthropic aren't trying to replace doctors—they're trying to give doctors their time back. By targeting administrative automation ($35B prior authorization burden) instead of clinical decision-making (Watson's fatal mistake), the 2026 healthcare AI race represents a fundamentally different strategic approach with measurable ROI.
Market Projection: $105B+ healthcare AI market by 2030 (7x growth from 2024)
In the first eleven days of 2026, the future of healthcare was rewritten. While headlines focused on AI "diagnosing" patients, the real story is far more strategic: a calculated race for a market projected to exceed $100 billion by 2030.
I've spent over 15 years building data products and AI platforms at companies like Best Buy and Target. I've watched technology promises come and go. I've seen the hype cycles. And I've learned to ask a simple question that separates real transformation from expensive experiments: What's actually different this time?
With healthcare AI, that question matters more than ever. The graveyard is well-populated. IBM Watson Health, once touted as the future of oncology, was sold for parts in 2022 after billions in investment yielded little measurable impact. DeepMind's protein folding work is impressive, but no AI-inspired drug has reached millions of patients yet.
So when OpenAI and Anthropic launched healthcare products within four days of each other in January 2026, my instinct was skepticism. But as I dug into the details, I found something genuinely different. Not in the technology itself, but in the strategy, the timing, and the problem being solved.
The 4-Day Sprint: What Actually Happened
The speed tells you everything about the stakes.
Consumer-facing product allowing users to sync personal health data from Apple Health, MyFitnessPal, and other wellness platforms.
Enterprise HIPAA-compliant API with hospital system integrations. AdventHealth, Boston Children's, Cedars-Sinai, HCA Healthcare, Memorial Sloan Kettering, Stanford Medicine, and UCSF announce deployment.
HIPAA-ready infrastructure with native connectors to CMS Coverage Database, ICD-10 codes, National Provider Identifier Registry, and PubMed.
The timing at J.P. Morgan was no accident. This is where healthcare executives, investors, and deal-makers gather. Anthropic wasn't just launching a product—they were positioning for a specific audience: the people who fund healthcare transformations and the executives who greenlight enterprise contracts.
Why IBM Watson Failed (And Why It Matters Now)
To understand why this moment is different, we need to understand why the last great healthcare AI bet collapsed.
In 2011, IBM's Watson won Jeopardy against human champions. IBM saw healthcare as the obvious commercial application. Watson would revolutionize cancer care by digesting medical literature, patient records, and treatment outcomes to recommend optimal therapies.
IBM invested over $5 billion in Watson Health through acquisitions alone. They employed 7,000 people at the peak. Ginni Rometty, IBM's CEO, called healthcare their "moonshot."
By 2022, Watson Health was sold to Francisco Partners for approximately $1 billion—a fraction of the investment. IEEE Spectrum reported that around 50 partnerships had been announced with major healthcare organizations. None had produced usable tools or applications.
Watson tried to replace physician judgment in complex clinical decisions—the "robot doctor" approach. But medicine doesn't work that way. Every patient is unique. Clinical guidelines conflict.
Watson couldn't read doctors' notes effectively. The unstructured, inconsistent nature of clinical documentation proved far harder than game show questions.
What would "success" even look like? Better outcomes? Faster diagnoses? Cost savings? Watson never had a verifiable metric.
IBM's marketing outpaced capabilities. When the gap became obvious, trust evaporated.
The lesson from Watson isn't that AI can't work in healthcare. It's that trying to replace physician judgment with AI is extraordinarily hard, maybe impossible with current technology. The wins will come from augmenting human capabilities in areas where the value is clear and measurable.
The Strategic Pivot: From Robot Doctors to Administrative Escape Hatches
Here's where OpenAI and Anthropic are doing something genuinely different.
They're not trying to replace doctors. They're trying to give doctors their time back.
Look at what Anthropic explicitly called out: prior authorization support, claims appeals, coverage verification. Look at what OpenAI highlighted: discharge summaries, patient instructions, clinical letters, administrative workflow assistance.
These aren't sexy features. They don't make for dramatic headlines about AI diagnosing diseases. But they target a real, measurable, enormous problem.
"Clinicians often report spending more time on documentation and paperwork than actually seeing patients."
— Mike Krieger, Chief Product Officer, Anthropic
This represents a fundamental strategic pivot. Instead of asking "Can AI make better clinical decisions than doctors?" (answer: unclear, maybe never), they're asking "Can AI handle the administrative burden that burns out doctors and delays patient care?" (answer: almost certainly yes).
The "Pajama Time" Problem: 35% of Physician Time Lost
Physicians have a term for the hours they spend at night finishing documentation and administrative work: "pajama time." It's the work that happens after the clinic closes, after dinner, after the kids go to bed.
The data is stark. According to American Medical Association studies, the average physician works a 57.8-hour week. Of that time, roughly 35% goes to indirect patient care and administrative tasks: documentation, prior authorization, claims paperwork, results review.
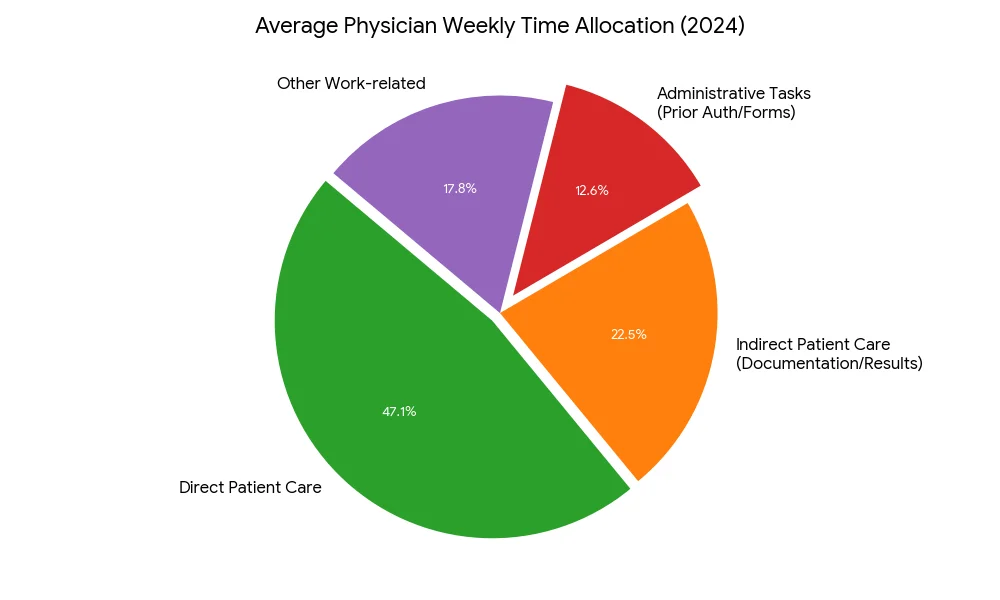
That's over 20 hours per week that a highly trained physician spends as a data entry clerk. Twenty hours that could be spent with patients. Twenty hours contributing to the burnout epidemic that's driving doctors out of medicine.
The immediate goldmine for healthcare AI isn't clinical decision support. It's administrative automation. When 35% of a physician's time goes to paperwork, the ROI on automation is obvious and measurable.
The $35 Billion Prior Authorization Opportunity
Let me explain why Anthropic specifically built connectors to the CMS Coverage Database and ICD-10 codes.
Prior authorization is the process where a doctor must get insurance company approval before providing certain treatments or prescribing certain medications. In theory, it controls costs. In practice, it has become a bureaucratic nightmare.
According to the 2024 AMA Prior Authorization Survey:
The total annual cost of prior authorization administration in the U.S. healthcare system is estimated at $35 billion, according to 2025 data from JAMA.
This is the "size of the prize" for any AI company that can solve this specific administrative friction. For a physician trying to get a treatment approved, Claude can now:
- 1. Look up the specific coverage requirements in the CMS database
- 2. Find the correct ICD-10 codes for the diagnosis and procedure
- 3. Pull relevant clinical guidelines from PubMed to support medical necessity
- 4. Draft the authorization request with all required documentation
What used to take hours of phone calls, fax machines, and waiting on hold can potentially be reduced to minutes. That's not hype. That's automation of a well-defined, rules-based process.
The Market Reality: $105+ Billion by 2030
The healthcare AI market is experiencing explosive growth. Multiple research firms project the market will grow from roughly $15-26 billion in 2024 to over $105 billion by 2030, representing a compound annual growth rate of approximately 38%.
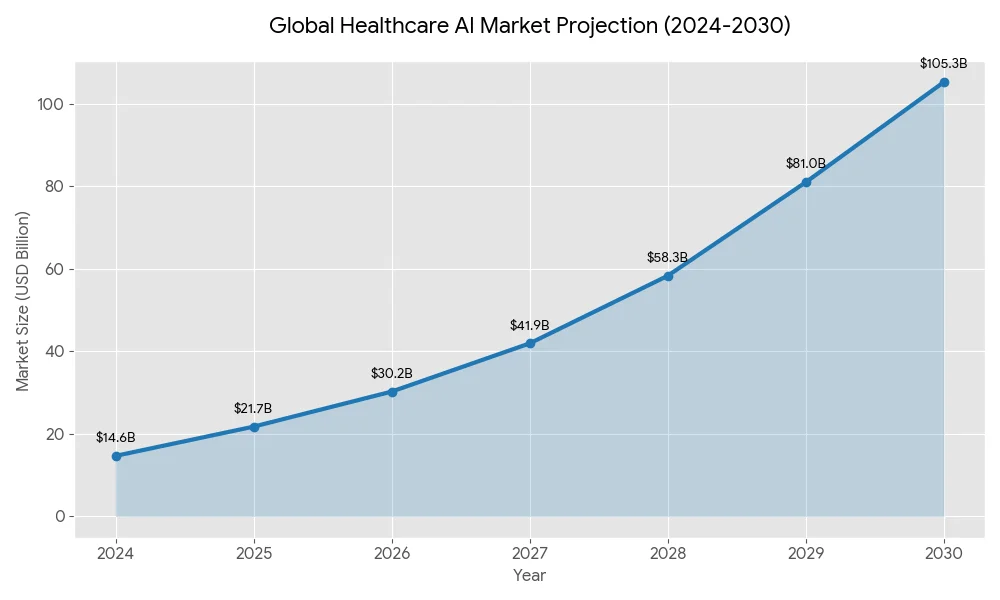
Some projections are even more aggressive. Strategy& (PwC's strategy consulting arm) estimates AI could enable an $868 billion opportunity in healthcare by 2030 when you include cost savings and revenue gains across the entire value chain.
The growth drivers are structural:
- • Aging populations increasing demand for healthcare services
- • Physician shortage creating need for productivity tools
- • Administrative cost crisis forcing automation adoption
- • HIPAA-compliant infrastructure now available from major AI providers
- • Proven ROI in specific use cases (ambient documentation, prior auth)
The IPO Narrative: Why Healthcare, Why Now
There's another dimension to this story that press coverage has largely missed: the IPO narrative.
Both OpenAI and Anthropic are approaching public markets. OpenAI's potential IPO has been discussed at valuations of $100+ billion. Anthropic's valuation has reportedly nearly doubled to $350 billion in recent months.
To go public successfully, you need more than "chatbot for consumers" or "API for developers." You need a story about becoming essential infrastructure for the economy's largest sectors.
Healthcare provides that story:
- • $4.5 trillion U.S. healthcare spending (18% of GDP)
- • Defensive market that grows regardless of economic cycles
- • Enterprise contracts with multi-year commitments
- • Regulatory moats that protect early entrants
If you want a thriving healthcare story for your public company narrative, you have to start early. You need existing partnerships with hospitals. You need healthcare data that's working. You need to be able to talk about millions of consumers benefiting from your product.
January 2026 was the time to start.
A Framework for Evaluating Healthcare AI
Based on this analysis, here's how I'd evaluate any healthcare AI investment or initiative:
Augmenting physician capabilities (administrative automation) = promising. Replacing physician judgment (clinical decision-making) = high risk.
Time saved per prior authorization = measurable. "Better patient outcomes" = too vague.
Prior authorization has defined rules and codes. Cancer treatment decisions involve infinite variables.
Administrative tools face lower regulatory hurdles than clinical decision support.
AI that drafts prior auth requests has clear human oversight. AI that recommends treatment is a liability minefield.
The Bottom Line: From Optional Tech to Critical Infrastructure
The January 2026 healthcare AI launches represent something genuinely different from the Watson era—not because the technology is radically better, but because the strategy is radically smarter.
OpenAI and Anthropic have learned from Watson's failures. They're:
- • Targeting administrative burden instead of clinical judgment
- • Building measurable ROI (time saved, costs reduced) instead of vague "better care"
- • Creating HIPAA-compliant infrastructure that reduces deployment friction
- • Positioning for enterprise contracts with clear governance features
For healthcare organizations, the question is no longer "Should we explore AI?" It's "How do we evaluate these competing platforms and deploy responsibly?"
For AI companies, healthcare is no longer an experimental vertical. It's critical infrastructure for the IPO narrative.
And for the physicians drowning in paperwork? January 2026 might be the moment their profession started to get its time back.

Evaluating Healthcare AI for Your Organization?
I help healthcare organizations and health-tech companies navigate AI strategy—from vendor evaluation to deployment roadmaps. Let's discuss how to avoid the Watson trap and focus on use cases with measurable ROI.
Schedule a Strategy Session